Rickets
Define: Rickets is a defect in mineralisation of the osteoid matrix that occurs before physical closure.
Features: clinically it is associated with
- Long bones
- Physical cupping
- Bowing
- Spine
- Codfish vertebrae
- Kyphosis
- Thorax
- Rachitic rosary
Pathology: Disruption of the normal Ca/Phos metabolism causes poor calcification in the Zone of Provisional Calcification can occur through a number of different mechanisms
- Nutritional deficiencies (Vitamin D common; Calcium and Phosphate rarer)
- Renal tubular defects and osteodystrophy
- GI absorption disorders
Vitamin D deficiency
Rarer now that Vitamin D is added to milk. Risk factors include prematurity, asian immigrants, and malabsorption.
Say
- Low Ca is sensed by chief cells which release PTH
- PTH acts to upregulate osteoclasts via OB differentiation, inhibiting OPG and increasing RANKL, but…
- Deficiency means feedback cannot act to increase 1,25 Vitamin D so strong signal for GI absorption is absent
- Net effect is that balance between PTH and Vitamin D is lost so that Ca is maintained by PTH (secondary hyperparathyroidism) action on the bone, presenting as rickets
Usually managed with dietary replacement of Vitamin D.
Draw
Low Vitamin D uncouples its effect from PTH which supports Ca at the expense of Phos

Calcium and phosphate deficiencies
Follow a similar pattern but are rarer.
In Ca deficiency, low Ca drives PTH (secondary hyperparathyroidism) and conversion of 25 Vit D to 1,25 Vit D. The biochemical findings are similar, with PTH driving raised Alk Phos, low serum Phos, low urinary Ca, but also depleting 25 Vit D stores.
In Phos deficiency, proximal tubule is stimulated to convert 25 Vit D to 1,25 Vit D and depleting its stores, but there is no PTH stimulus so no secondary hyperparathyroidism.
Hereditary Vitamin D dependent rickets
Similar feaures to Vitamin D deficient rickets, but tends to be more severe and associated with total baldness. There are two types with an analgous aetiology to diabetes type 1 & 2:
- Type 1 is caused by reduced production of 1,25 Vitamin D due to a defect in 1-alpha hydroxylase.
- Type 2 is caused by insensitivity to 1,25 Vitamin D due to a receptor mutation.
Say - Type 1
- Type 1 is an autosomal recessive mutation in the 1 alpha hydroxylase gene
- 1,25 Vitamin D dependent Ca homeostasis cannot occur
- This drives a secondary hyperparathyroidism
- Consequent imbalance in net effects of PTH and Vitamin D, which tends to present more severely than pure dietary Vitamin D deficiency.
Treatment is by oral supplementation of activated 1,25 Vitamin D at physiological doses (1-2 microgram per day)
Draw - Type 1

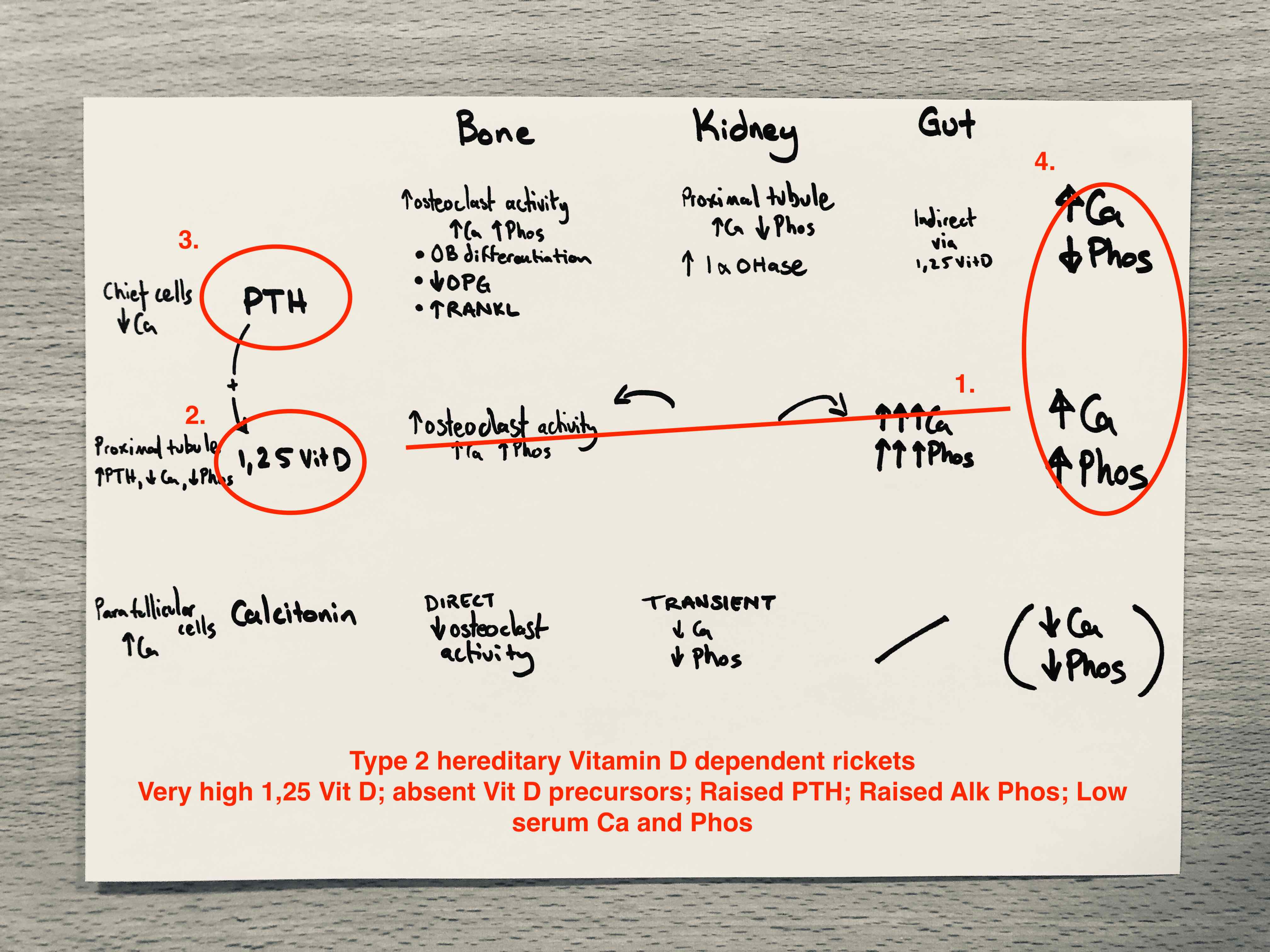
Say - Type 2
- Type 2 is also autosomal recessive, but affects the 1,25 Vitamin D receptor, blocking its end organ effects
- Loss of negative feedback drives significantly raised 1,25 Vit D levels and a fall in precursors
- These are ineffective at maintaining serum Ca and Phos which stimulates PTH
- The net effect is very high levels of activated Vitamin D with low serum and urinary Ca
Treatment is high dose Vitamin D with elementary calcium.
Draw - Type 2